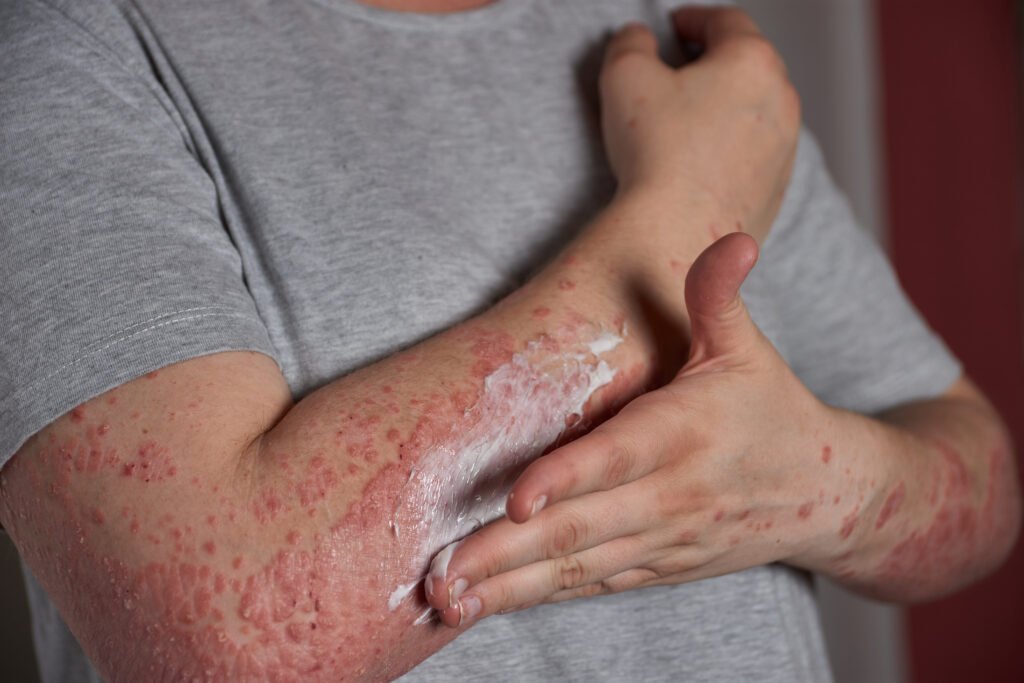
The itch arrives first, before any visible sign betrays it. You scratch absently, then with increasing urgency, until the skin reddens and rises into welts that weep and crust. The cycle repeats through sleepless nights: itch, scratch, damage, repeat. In the morning, your sheets bear traces of blood and skin flakes. The visible rash draws questions from strangers, pitying looks, assumptions about contagion or hygiene. You have explained a hundred times that no, it is not contagious, yes, you have tried that cream, no, it is not just dry skin.
Eczema, or atopic dermatitis, affects millions worldwide, yet remains misunderstood as a minor cosmetic concern rather than the chronic, burdensome condition it truly is. Understanding its mechanisms, triggers, and treatment options transforms management from frustrating trial-and-error to strategic control.
Understanding Eczema’s True Nature
Eczema represents a complex inflammatory skin condition with genetic, immune, and environmental contributors, not a simple moisture deficiency or allergic reaction.
The skin barrier breakdown
Healthy skin maintains a protective barrier of lipids and proteins that prevents water loss and blocks irritants, allergens, and microbes. In eczema, genetic variations, particularly in the filaggrin gene, compromise this barrier. Filaggrin helps structure the outer skin layer; its deficiency creates microscopic cracks through which moisture escapes and triggers enter.
This “leaky” barrier initiates inflammation. Immune cells respond to perceived threats, releasing cytokines that drive redness, swelling, and itching. The itch-scratch cycle further damages skin, perpetuating inflammation and sometimes introducing infection through broken skin.
The atopic march connection
Eczema often represents the first manifestation of atopic disease. Many patients later develop allergic rhinitis and asthma, the so-called “atopic march.” Shared genetic and immune mechanisms link these conditions. Early, aggressive eczema treatment may reduce subsequent atopic disease development, though this remains under active investigation.
Distinguishing eczema from mimics
Contact dermatitis produces similar appearance but results from specific external exposures and resolves when these are identified and avoided. Psoriasis features thicker, silvery-scaled plaques with different distribution patterns. Seborrheic dermatitis affects oil-rich areas with greasy scaling. Fungal infections, scabies, and cutaneous T-cell lymphoma occasionally mimic eczema, requiring biopsy for differentiation when presentation is atypical.
Recognizing the Full Symptom Spectrum
Eczema manifests differently across age groups and body sites, though core features remain consistent.
Infantile presentation
Onset typically occurs between two and six months. The face, particularly cheeks, shows red, weeping patches that crust and scale. The scalp may develop thick, yellowish scale resembling cradle cap but more inflammatory. Diaper area is usually spared, distinguishing eczema from irritant diaper dermatitis. Infants are restless, sleep poorly, and may show failure to thrive if severe.
Childhood and adult patterns
As children age, eczema often migrates to flexural areas: antecubital fossae, popliteal fossae, wrists, and ankles. Lichenification, skin thickening from chronic rubbing, develops. Adults may show hand dermatitis, eyelid involvement, or nummular patterns: coin-shaped plaques on extremities.
The itch that defines the disease
Pruritus represents the hallmark symptom, often described as unbearable and worse at night. Scratching provides momentary relief but damages skin, introducing infection and perpetuating inflammation. Sleep disruption from itching affects quality of life profoundly, contributing to behavioral problems in children and work impairment in adults.
Secondary complications
Bacterial infection with Staphylococcus aureus occurs frequently, indicated by honey-colored crusting, pustules, or sudden worsening. Herpes simplex virus can cause eczema herpeticum, a serious disseminated infection requiring urgent antiviral treatment. Chronic rubbing produces lichen simplex chronicus: permanently thickened, leathery plaques with exaggerated skin lines.
Building an Effective Treatment Strategy
Eczema management requires multimodal approach addressing barrier repair, inflammation control, trigger avoidance, and infection prevention.
Foundation: skin barrier restoration
Emollient therapy forms the cornerstone, applied liberally and frequently. Ointments, with minimal water content and no preservatives, provide superior barrier protection but feel greasy. Creams offer acceptable compromise for many. Lotions, with higher water content, prove inadequate for significant disease.
Application timing matters: within three minutes of bathing, when skin remains slightly damp, optimizes moisture retention. Bathing itself, contrary to old advice, benefits when done properly: lukewarm water, fragrance-free cleansers, limited duration, immediate emollient application.
Anti-inflammatory therapy
Topical corticosteroids remain first-line for flares, with potency matched to severity and location. Low-potency options (hydrocortisone) suit face and skin folds; mid-potency (triamcinolone) for trunk and extremities; high-potency (clobetasol) for lichenified plaques, limited duration. Fear of side effects, including skin thinning and systemic absorption, leads to underuse; when applied appropriately, these risks are minimal compared to untreated disease burden.
Topical calcineurin inhibitors (tacrolimus, pimecrolimus) provide steroid-sparing options for sensitive areas and maintenance therapy. They sting initially for some patients but lack steroid side effect profile.
Advanced and systemic approaches
Phototherapy with narrowband UVB benefits widespread disease unresponsive to topicals. Dupilumab, a biologic targeting IL-4 and IL-13, revolutionized moderate-to-severe eczema treatment, providing dramatic improvement for many previously uncontrolled patients. Other biologics and JAK inhibitors expand options for refractory disease.
Systemic immunosuppressants (cyclosporine, methotrexate, azathioprine, mycophenolate) retain role for severe cases, with monitoring for toxicity. These require specialist management.
Trigger identification and avoidance
Common triggers include fragrances, harsh detergents, wool and synthetic fabrics, temperature extremes, sweating, stress, and specific allergens. Patch testing identifies contact allergens when standard therapy fails. Food allergies trigger eczema in minority of patients, particularly infants; elimination diets require careful guidance to avoid nutritional deficiency.
Conclusion
Eczema imposes burdens extending far beyond skin appearance: sleep disruption, psychological distress, social stigma, and infection risk. Yet with proper understanding and comprehensive management, most patients achieve meaningful control.
If you or your child struggles with eczema, seek dermatology or allergy specialist evaluation for severe or refractory cases. Do not accept dismissal as “just dry skin” or incomplete treatment with weak steroids alone. Modern therapeutic options, including biologics, offer genuine transformation for previously suffering patients.
The goal is not cure, which remains elusive, but sufficient control to allow normal sleep, unrestricted activity, and freedom from constant itch awareness. That goal is achievable for most, and worth pursuing through systematic, informed management rather than resigned suffering.